The healthcare organizations are in a highly regulated business in the United States of America. With the changing reimbursement models and the heightening payer scrutiny, comfortable control of billing and coding procedures is now a necessity rather than a choice towards financial stability and legal safeguards.
Revenue cycle management compliance will make sure that providers comply with the regulations expected of them, in addition to realizing the full value of the services they offer.
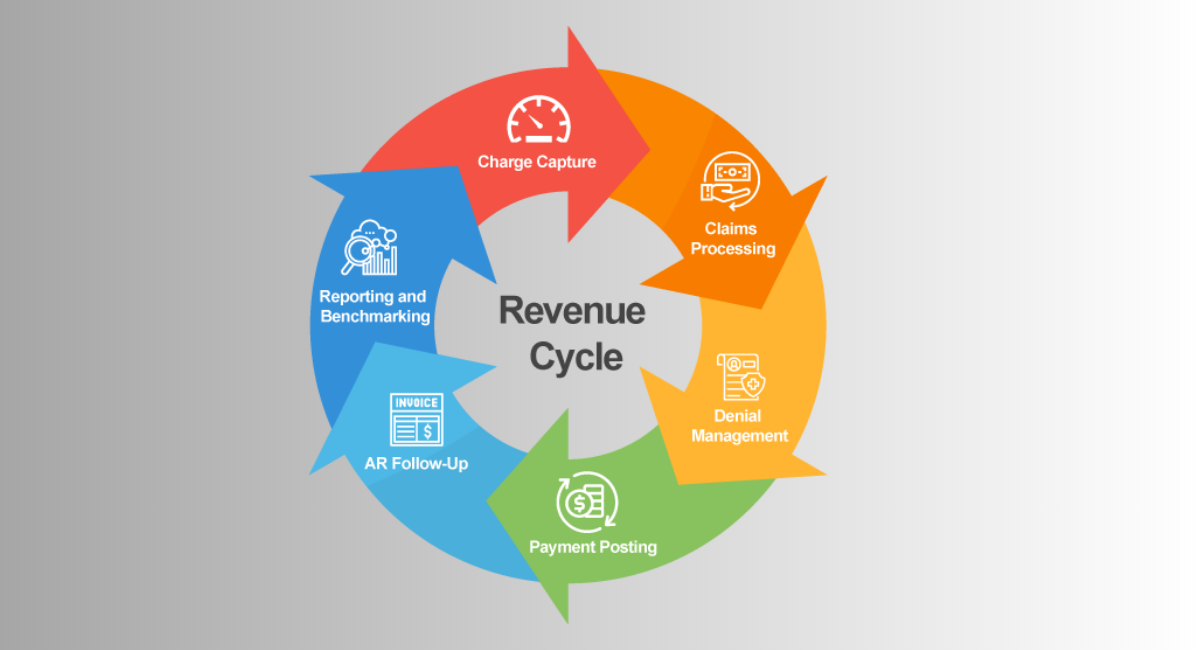
Revenue cycle management (RCM) cuts across all the administrative and clinical points of contact between patient registration and final payment. In this cycle, compliance depends on proper documentation, correct coding, timely filed claims, and compliance with federal and payer-specific regulations. Any mistakes in the process will result in claims being denied, reimbursement delays, audits, or financial fines. Even minor inaccurate coding can have a major effect on the bottom line of an organization, as well as make it vulnerable to compliance risk in the federal fraud and abuse regulations.
The healthcare management receives regulations such as the Centers of Medicare and Medicaid Services (CMS) and the Office of Inspector General (OIG), which expect providers to exercise proactive supervision. This involves the practice of internal audits, standardized coding procedures, and healthy documentation practices. Nevertheless, the growing complexity of the payer policy and the frequent changes in the coding make it hard to oversee manually. With the increasing clinical workloads, providers might miss the opportunity of charge capture unintentionally or give incomplete claims.
Leveraging the right technology can transform compliance and financial operations. For a deeper look at how digital tools accelerate efficiency and growth, read about technology for business growth.
The Compliance Issues in Charge Capture.
Charge capture is among the weak points of the revenue cycle. It obligates clinicians to record the services delivered, the performed procedures, and the resources used correctly. Any small lapse in documentation can lead to undercoding, overcoding or rejection of claims. Undercoding contributes to loss of revenue, whereas overcoding can attract payer audits and compliance reviews.
The processes of charge capture will be manual and will be dependent on the accuracy of the human and the timeliness of the documentation. Clinicians in high-pressure health care settings, especially within specialty practices and within hospital settings, tend to experience time pressure that may result in missed or delayed entries. The administrative teams are then forced to resolve differences, which adds to the cost of operations and delays in the reimbursement process.
Also, the constant changes in the payer guidelines and changes in the coding rules pose continuous compliance risks. Organizations will not be able to keep up without real-time updates and smart validation systems. This is where compliance management is being transformed due to the use of technology.
The way AI Empowers Revenue Cycle Oversight.
To lower risk and increase efficiency, artificial intelligence is progressively being incorporated in revenue cycle activities. The systems, which are based on AI, are able to analyze clinical documentation in real-time, identify inconsistencies, and propose suitable codes in accordance with the existing regulatory standards. Organizations eliminate the use of manual review in validation checks through automation, as well as minimizing unnecessary errors.
An example of AI Charge Capture is the solution of Claimocity. The platform, which was designed to assist providers during the point of documentation, will increase compliance levels with revenue cycle management by detecting coding discrepancies prior to claim submission. Rather than finding problems once the payment is denied, the providers have the opportunity to spot and eliminate mistakes proactively.
The AI engine examines documentation patterns, compares them to coding standards and makes sure that services provided are captured accordingly. This eliminates underbilling and overbilling risks as well as enhancing internal compliance security. Compliance can be made an application of intelligence instead of an addition or upgrade by integrating intelligence into workflow processes.
Enhancing Accuracy of Billing and Risk Minimization.
The accuracy of billing has a direct bearing on the performance of an organization. Claims that are denied need to be reworked, use administrative resources and slack cash flow. More to the point, recurring errors are open to regulatory review. AI-assisted charge capture software can assist in making sure that claims are incurred in accordance with documentation and payer needs at the beginning.
The approach of Claimocity fits in the clinical workflow smoothly without causing friction to the provider, but its compliance integrity is intact. The system aids in the correct selection of codes and also verifies that the documentation is complete before it is submitted. This enhances the first-pass enhancement of claims besides audit readiness.
Transparency and accountability are also enhanced by accurate documentation. Organizations that have implemented AI-validated charge capture processes can exhibit organized compliance measures in case of a payer review or an audit. This is a proactive stance that minimizes the exposure of financial liability and enhances institutional credibility.
Ethical Support of Sustainable Financial Performance.
Compliance is not merely the process of escaping punishment but developing a strong financial base. Having invested in smart compliance systems, healthcare organizations are placed in the position of sustainable growth. Increased accuracy of billing has resulted in predictable revenues, decreased administrative workload, and increased efficiency in operation.
Providers can understand the revenue trends and possible risk areas better by taking advantage of AI-powered charge capture. The information formed by these systems can be used in training programs, workflow restructuring, and policy changes. Such cycle of continuous improvement helps maintain regulatory compliance as well as long-term profitability.
Besides, the integration of the latest compliance technologies is an indication of being a responsible ruler. Healthcare organizations are being subjected to increased demands to deploy contemporary safeguards that ensure financial integrity by patients, payers, and regulatory bodies. The compliance strategies with the help of AI meet these expectations and build a stronger trust among stakeholders.
The Future of Revenue Cycle Manager Compliance.
With the increasing complexity of healthcare reimbursement systems, manual procedures will no longer be enough. Smart systems should be incorporated in the organizations such that they do not interfere with the clinical care but generate more oversight in the organization. The AI Charge Capture of Claimocity is a futuristic product that attempts to integrate its compliance checks directly into the revenue cycle operations.
The strategy of proactive compliance management in the contemporary regulatory environment is a compulsory requirement. Enhancing the compliance of revenue cycle management with AI-based tools is not only the way of minimizing the number of coding mistakes and increasing the quality of billing, but also the means to protect the reputation and financial results of the organization. It is through the adoption of the modernized charge capture technology that the medical practitioners can confidently sail through the regulatory requirements and optimize revenue potentials in an increasingly competitive environment.